On Easter weekend in 2014, mom Suzie Veillette made a small concession for her kids that would change all of their lives forever.
The bit of surrender came in the form of a Reese’s Peanut Butter Egg.
“We had just finished dinner and my oldest one begged, ‘please let us have some of our Easter candy for dessert,’” Veillette said.
She agreed and intentionally picked up the Reese’s candy because she believed it would be easy for her son Liam, then 1½, to chew.
“So we gave it to him and within two bites, I mean it was quick, he started breaking out around his mouth and he started rubbing his throat,” she said. “I knew immediately he was having a food allergy.”
According to the Food Allergy Research and Education (FARE) organization, nearly six million children – that’s one in 13 kids or two kids in every classroom – have food allergies.
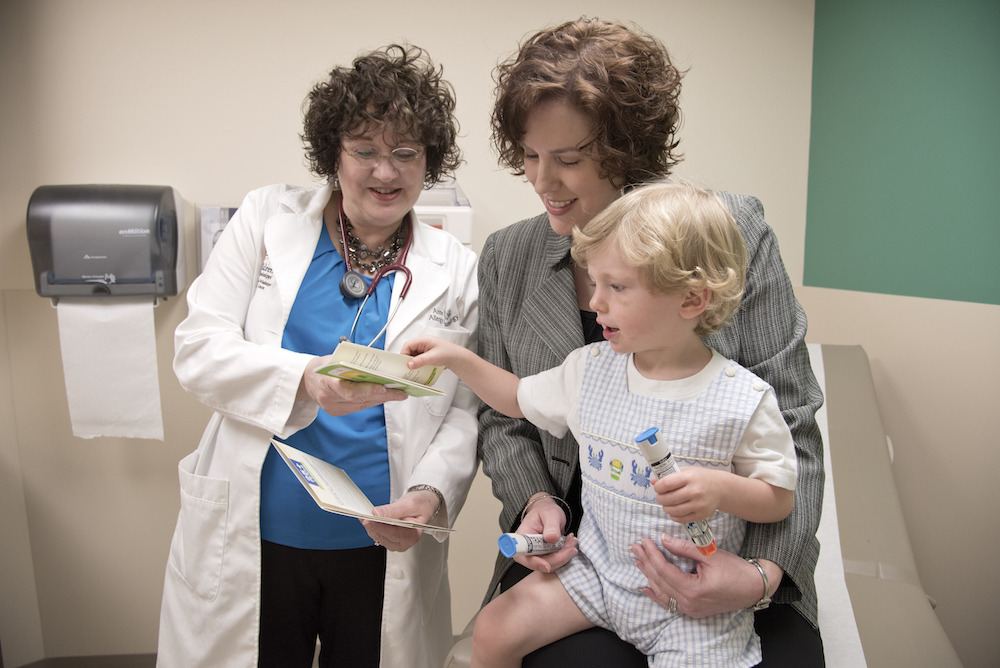
Dr. Anne Yates, professor of pediatrics and medicine and chief of the Section of Allergy and Immunology in the Department of Pediatrics, said a reaction to a food allergy can vary widely from an eczema flare, hives and itching, swelling of the face, to vomiting and diarrhea.
More severe symptoms include wheezing, shortness of breath, throat swelling, or cardiovascular symptoms also known as anaphylactic shock, where blood pressure drops. Death is a possibility and minutes count.
Symptoms – even the more severe ones – can begin less than five minutes after a child comes into contact with the food.
“With mild symptoms, just a little bit of hives, itching, or skin swelling, you can give Benadryl and watch closely,” Yates said. “If the hives or swelling worsens or if the child is having any breathing difficulty or feeling weak or faint, then you have to give epinephrine and call 911 for the ambulance to take them to the hospital because it could get worse and become deadly.”
And it did get worse for Liam, after it got a little better.
Veillette, a licensed nurse, got out the Benadryl and called the on-call nurse at her pediatrician’s office who told her to call 911.
When the paramedics arrived, the Benadryl had kicked in and Liam seemed ok. They told her she did the right thing and to go ahead and put Liam to bed.
Once they left, though, Liam’s condition worsened. He began screaming inconsolably and developed a total body rash.
In retrospect, Liam should’ve been given epinephrine, but the Veillettes didn’t have epinephrine, much less know he needed it.
Instead, they drove Liam straight to the emergency department at Batson Children’s Hospital.
Luckily, Liam improved without the epinephrine. Doctors were able to treat him with steroids and hours later, released him with a diagnosis of suspected allergy to peanuts.
The diagnosis was later confirmed by blood tests that also showed Liam was allergic to the part of the protein in peanuts that carries a higher risk for anaphylactic shock.
That’s when Veillette began researching food allergies and started to comprehend how dangerous his condition really was.
“It’s completely changed our life,” Veillette said, recalling the events of that week. “It’s a little easier now because I’ve had a year to deal with it, but every day I drop him off at school and I get that thought in my head, ‘Am I going to get that phone call today?’”
She has become somewhat of a food allergies expert since her son’s diagnosis and worries about the lack of understanding, something she experienced firsthand.
And indeed, what is known about food allergies and what is unknown are about equal.
- We know reactions can get more severe with repeated exposures, but we can’t anticipate what the reaction will be – even in one individual. It’s entirely possible Liam may indeed need epinephrine next time.
- We know food allergies are on the rise in children, with a 50% increase between 1997 and 2011 according to the Centers for Disease Control, but we don’t know why. As Veillette says, “If you don’t know someone with food allergies, you will.”
- We know 90 percent of food allergies are to eight foods – milk, egg, peanuts, tree nuts, wheat, soy, fish, and shellfish – but we don’t know what causes people to develop the food allergies.
And since we don’t know what causes them, there is no cure. The only option for those affected is total avoidance.
That means more than not giving her son a peanut butter sandwich, says Veillette.
“That’s another misconception,” she said. “It’s not that easy because it’s hidden everywhere.”
In 2004, the Food and Drug Administration passed the Food Allergen Labeling and Consumer Protection Act, which requires the eight most prevalent food allergens to be listed on all packaged food labels in clear language – “May contain: peanuts.”
The problem is, the requirement only applies to packaged foods and the top eight often show up in unexpected places.
Veillette cites peanut oil in sunscreen, fish oil in baby food, milk in non-dairy creamer, and wheat in paste, as some examples. Yates added that something as innocuous as potting soil probably contains peanut shells.
Couple that with the fact that many consumers aren’t reading food labels to discover the hidden offenders. Even if they are, the non-packaged foods — sunscreens and paste — list them under other, less obvious names. Arachis oil is another name for peanut oil.
“I have to read every label on everything every single time,” she adds.
That’s where Yates comes in. Aside from testing for and diagnosing food allergies, she and her colleagues help families with the only weapon one really has in this fight – proper planning.
So after a family receives the diagnosis telling them what the child can’t eat, Yates helps them figure out what they can eat.
“We try to help them out with making sure they’re getting a balanced nutritious diet. And sometimes we consult with a dietitian at Children’s to help out with meal planning and making sure they’re getting good balanced foods,” she said.
She also teaches parents how to use an epinephrine injector. The Veillettes now have more than one.
Yates helps them develop a written-out anaphylaxis treatment plan in case a child accidently ingests a food allergen.
Liam’s plan is “plastered on the wall” at his daycare, where Veillette also presented a PowerPoint presentation on dealing with food allergies to all the teachers.
As for the Veillettes, every time they leave the house, they have to plan – whether it is for school or a birthday party or dinner at a restaurant or an Easter egg hunt.
“Even though I feel like we have a plan now, with each age and each new experience, it’s something new that we have to deal with,” Veillette said.
She’s also become committed to the cause of spreading the word about the dangers of food allergies, so other parents won’t be caught unawares.
“There’s this perception that they’re not that big of deal; that we’re blowing this out of proportion,” she said. “But this is a medical condition and its life-threatening and we’ve got to treat it as such.”
Courtesy University of Mississippi Medical Center
Recent Comments