
Several times each day, Willie Haynes (BSES 08) sees the sacrifices made by a population that is pushing toward reaching its full potential. Meaningful moves forward occur in 60-minute increments for Haynes and the wounded warriors at Walter Reed National Military Medical Center in Bethesda, Maryland.
As a traumatic brain injury specialist and occupational therapist, Haynes starts his mornings with a daily schedule that is broken down into one-hour treatment sessions.
“It’s important for people to understand the sacrifice our wounded warrior population gives,” Haynes says. “It’s interesting to see the wounded warriors’ determination and their ability to adapt to any situation.”
The situations that Haynes evaluates include patients with any sort of neurological deficit or movement issue caused by issues such as battlefield injuries, motor vehicle accidents, stroke and multiple sclerosis. When a patient is dealing with a neurological disease or disorder, Haynes steps in with a two-part remedy. He works on improving physical strength, balance and mobility as well as sharpening a wide range of cognitive skills.
“I do a lot of cognitive rehabilitation working with traumatic brain injury patients,” Haynes says. “We work on short-term memory, long-term memory, reading comprehension skills and life skills.”
That includes working on basic functional components of everyday living.
“Can a patient process information they are receiving functionally?” Haynes asks. “Can a person read the instructions on a recipe and follow them?”
As a patient tackles those sorts of tasks in a kitchen, Haynes is focused on details such as problem solving and the patient’s personal safety. It’s all part of a process that also depends on an individual’s place on the functional spectrum.
“I might have a low-functioning patient who needs a maximum amount of verbal cues,” he says. “I am trying to draw them to a place where they can process what I am asking them to do. Another stroke or traumatic brain injury patient might have more movement disorders. They might not have the balance to stand and wash their hands or move around.”
Many incidents can lead to head trauma and a traumatic brain injury. It may be a battlefield injury or an emergency situation much closer to home. Every day, 153 people die from injuries that include a traumatic brain injury component, according to the Centers for Disease Control and Prevention. Traumatic brain injuries contribute to about 30 percent of all injury-based deaths. Falls are the leading cause of these injuries, accounting for nearly half of all TBI-related emergency department visits.
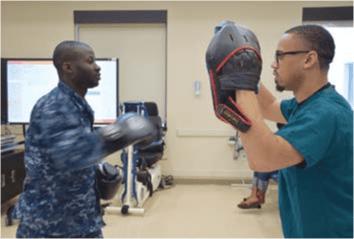 For occupational therapists who work in densely populated metro areas, the details of a TBI can run the gamut from a fall to a fistfight to a gunshot-wound victim.
For occupational therapists who work in densely populated metro areas, the details of a TBI can run the gamut from a fall to a fistfight to a gunshot-wound victim.
Shawn Phipps is the chief strategic development officer at Rancho Los Amigos National Rehabilitation Center in Los Angeles. Calculating the damage done by gunshot wounds is part of the process in many cases from Los Angeles to Washington D.C.
“The medical complexity of traumatic brain injury is similar at Walter Reed and on the West Coast,” Phipps says. “That blast from a gunshot wound often penetrates the entire brain. We are helping patients gain function in all sections of life. There are often cognitive and psychological issues. You are dealing with the physical and mental aspects of helping that person get to the highest level of life possible.”
Rancho Los Amigos National Rehabilitation Center serves a dual purpose. In addition to the patient treatment aspect, the facility also functions as a teaching hospital. In that respect, the most challenging cases provide educational tools for occupational therapists in training. Phipps says Rancho Los Amigos and Walter Reed are both great training grounds for students.
“It gives you an opportunity to treat the worst of the worst,” he says. “Clinicians help those students learn from seeing how those injuries present. Students go back to school, and they benefit from that teaching.”

Many of those opportunities to assist patients on the journey to reaching their highest quality of life come from the medical advances that have enabled more patients to be saved in operating rooms before they reach the care provided by occupational therapists.
“Fifty years ago, many of these patients would not have survived,” Phipps says. “Now with the medical technology we have … having the benefit of keeping people alive and keeping them well is unbelievable even after a severe injury.”
OT Experience in Ghana

Part of Haynes’ education as an occupational therapist happened 5,800 miles away from his hometown of Louisville, Mississippi. Haynes is a program manager for an outside non-profit organization that helps provide access to rehabilitation services for people with disabilities in developing countries. A couple of co-workers and Haynes were interested in providing occupational therapy abroad. One of those friends has family from Liberia. She started traveling and doing volunteer work for rehabilitation clinics, which set the stage for Haynes to help children and their families in West Africa.
“She came back with the idea of doing her own thing, and she reached out to me,” Haynes says. “She developed the program, and we helped her with carrying out the mission.”
That took Haynes to Ghana on his first rehabilitation mission trip. The destination was a teaching hospital in Cape Coast. Although the hospital facilities were well established, the concept of occupational therapy was new to the area. Haynes and his peers provided assistance and served as mentors for a local, recent occupational therapy graduate.
Haynes worked in pediatrics, helping kids with feeding, swallowing and their physical movements and positioning. He and the team members also donated toys to add some fun to the treatment and help keep the kids engaged along the way.
Aside from those clinical interactions with the young patients in pediatrics, Haynes navigated occasional language barriers with the help of the other members of the hospital staff to communicate with parents and other family members.
“It was a very awakening experience for me,” he says, “mostly because they valued our opinions and our time and our presence. I remember walking into the clinic on the third day and a child I had treated on the first day. His mom had traveled to the Cape Coast area. She was asking questions and had waited to see us. I appreciated that. [Patients’ families] were open to new ideas. Not to say that we don’t do that in the U.S., but it was just coming from a different perspective. They treated me like family. They trusted me with their child.”
Before Haynes experienced that career and personal growth in Ghana, he took early steps on that journey in Oxford while pursuing a bachelor’s degree in exercise science. Interacting with fellow students through the University Judicial Council, Alpha Phi Alpha Fraternity and the National Pan-Hellenic Council Executive Board contributed to Haynes becoming an INROADS scholar. Haynes took courses during his sophomore year that showed him the differences between physical and occupational therapy and how aspects of occupational therapy fit well with his career passions.
“Ole Miss prepared me for the world,” Haynes says. “Being a young man, the university taught me to embrace people from all walks of life; it taught me how to network and give back to the community. I am still talking to people — different professionals — from all walks of life.”
Independence Day

Haynes carries those moments with him during his daily appointments with wounded warriors at Walter Reed. The level of independence for an individual depends on where he or she falls on the injury scale. For some, being able to spend four hours independently before a caregiver arrives is a big step. Others are aiming to live on their own and return to school or a job. Seeing those goals met provides perspective for Haynes.
“It’s challenging, and it teaches me how to be flexible and communicate effectively,” Haynes says. “It teaches patience and determination. The work made me more open to challenges. Regardless of what I encounter, there can be no excuses when it comes to every day.”
Evaluating a patient’s ability to take on a new challenge sometimes involves teaming up with other departmental staff members at Walter Reed. The summer climate in Maryland provides opportunities for patients to pick flowers, plant vegetables or maintain gardens. Winter months can mean a more strenuous test for some patients.
“We might team up with the recreational department to do adaptive skiing,” Haynes says. “Can this person balance and learn a new skill?”
Closer to home, Mississippi residents who are navigating their own roads to recovery after a traumatic brain injury often rely on guidance from the Brain Injury Association based in Jackson. For those patients, working up to being able to do a few hours of rehabilitation a day is part of the process of being cleared to either go to a post-acute inpatient rehab facility or being able to return home.
Because there is not a post-acute residential rehab facility in Mississippi, the treatment plan often includes patients going to Louisiana or other neighboring states. House Bill 478, which defines a post-acute residential brain injury rehab facility for licensing purposes, passed a House vote in January and a Senate vote in March before it was signed and approved. It went into effect on July 1.
“Hopefully, in the next year, we will have a post-acute facility,” says Lee Jenkins, executive director of the Brain Injury Association of Mississippi. “A lot of times,family members of patients will call us and ask where they should go now. We act as a facilitator for families and try to hook them up to rehab services.”
The association also assists people with spinal cord injuries. Sometimes, the nature of a brain injury can make the need for assistance less apparent to casual observers.
“There is a little more available for people with a spinal cord injury,” Jenkins says. “Sometimes a brain injury is an ‘invisible injury.’”
That “invisible injury” can show up at home or abroad on a battlefield. With a mild traumatic brain injury (or concussion), although the initial symptoms can appear to be relatively mild, a range of issues can persist if left undiagnosed and untreated.
“From the wars in Afghanistan and Iraq, we have seen unique blast injuries,” Phipps says. “There is a high incidence of mild traumatic brain injury. It is less obvious than a gunshot [injury].”
It is all part of the spectrum of patient injuries that Haynes has witnessed since his arrival at Walter Reed three years ago, and it is a team effort.
“We converse back and forth as departments,” Haynes says. “When you see people doing great work, it motivates me. … I encourage people to go into occupational therapy. It brings about pride and a sense of responsibility. I am happy to say I am an occupational therapist, and I work at a great institution with wounded warriors and active duty military personnel.”
By Brian Hudgins
This story was reprinted with permission from the Ole Miss Alumni Review. The Alumni Review is published quarterly for members of the Ole Miss Alumni Association. Join or renew your membership with the Alumni Association today, and don’t miss a single issue.
For questions, email us at hottytoddynews@gmail.com.
