By Andrea Wright Dilworth
UMMC communications
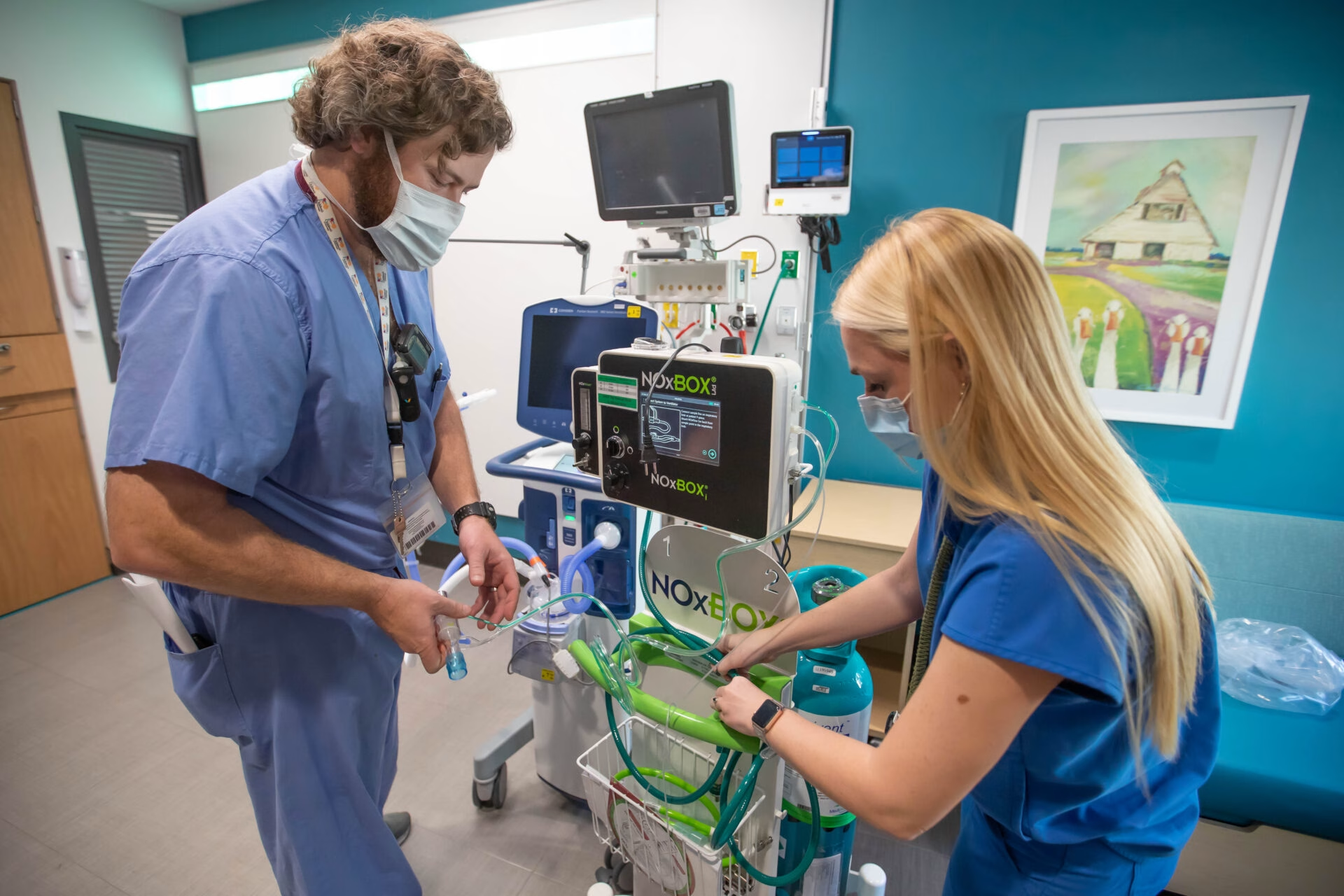
Hospitals across the state are caught up in yet another battle of supply and demand, and this time it’s not machines, gear, or even nurses. Instead, UMMC is one of many working feverishly to recruit and retain qualified respiratory therapists.
Respiratory therapists are trained to provide specialized care for patients who are having difficulty breathing on their own. They evaluate patients through diagnostic lung testing, chest exams and blood specimen analysis to recommend the best treatments to physicians, which include ventilators and other artificial airway devices.
Unfortunately, the pandemic has caused a shortage in respiratory therapists. Brady Holder, interim director of respiratory care, ECMO and associated clinical programs at UMMC, said he has talked with other department heads across the state, all of whom are having difficulty finding staff as the industry contends with “burnout,” the cost of having fewer respiratory therapists on staff to treat the sickest of patients.
“Staff numbers and the inability to hire respiratory therapists is my largest indicator,” explained Holder. “We have seen several staff members retire or retire early. We have also had one or two leave the profession completely.”
UMMC has therefore had to find ways to compete. “We are currently offering increased pay options through relief contract positions, bonus pay for extra shifts, as well as working with outside staffing agencies to find qualified staff,” he explained.
Yet, they’re competing with a formidable opponent: The travel market, which Holder said pays respiratory therapists “anywhere from 2 to 5 times what their standard salary would be depending on the location, type of contract and if they have any specialty experience — pediatrics, transport, acute care, ECMO.”

Holder calls the travel market the primary “driving force” behind the increase in pay. Though it has been recruiting respiratory therapists for some years now, taking an assignment meant having to move either to the West Coast or the Northeast. But in today’s market, respiratory therapists can take on assignments within hours, even minutes, from home, and UMMC has lost some therapists as a result.
Robert Mashburn, who has worked 17 years at UMMC – 15 as a respiratory therapist and two before that as an emergency room technician — knows he could earn more money elsewhere but has no intention of leaving. And he has his reasons.
“I feel like I make a difference, I enjoy the work I do,” said Mashburn, who now serves as clinical coordinator of respiratory therapy.
Dr. Driscoll DeVaul, who served as the director of respiratory care, ECMO and associated clinical programs before becoming assistant dean of academic affairs for the School of Health Related Professions in August, said recruitment efforts – many held virtually – have increased despite the pandemic, as UMMC has strengthened contacts with directors of respiratory therapy schools in the state and most recently ventured into Arkansas to recruit.
“The demand for RTs is a boost for the profession but also a concern for hospitals like UMMC,” DeVaul explained. “With COVID-19 being a respiratory disease caused by an airborne virus, respiratory therapists have been relentless in demonstrating their expertise in pulmonary physiology and respiratory diseases, which has ultimately proven very beneficial in caring for COVID-19 patients.
“The impact of respiratory therapists to health care is largely felt in the caring of premature babies with immature lungs, heart attack and stroke patients, and patients living with asthma and other chronic pulmonary conditions.”
DeVaul said hospitals must remain committed in the investment in respiratory therapists as critical members of the health care team because understaffing of the specialized health care practitioners can severely compromise the ability to provide optimal care and the promotion of improved patient outcomes.
Only a handful of community colleges in the state offer the two-year respiratory therapy program, said Holder, and they graduate relatively small classes each year, which makes it all the more challenging when trying to replace those who have left the profession.
“I reached out to a director at one of the local schools we work closely with,” Holder said. “She said that they are beginning to get more applications now. The biggest issue is finding qualified applicants. She said that they may receive 50-60 applicants, but only 25-30 may meet all the requirements to enroll into the program.”
Most programs in the state require an ACT score of 18 or higher, a C or better in prerequisite college courses, and a background check. No state institutions currently offer a bachelor’s degree in the field.
DeVaul, who just transitioned from practitioner to academics this year, said he continues to lend his years of experience and expertise to the respiratory care program, as needed.
“Breathing is fundamental to life, and respiratory therapists live by the motto: ‘Our work is so important, we are wired with the belief that if you are not breathing, nothing else matters; it doesn’t matter what kind of drugs, blood, or other medical interventions are given, we want to give our patients the best chance possible, the best respiratory care possible’,” said DeVaul.
“SHRP looks forward to future collaborations with UMMC’s adult and children’s respiratory departments, as well as other related programs, as we work to recruit and retain a strong clinical workforce.”